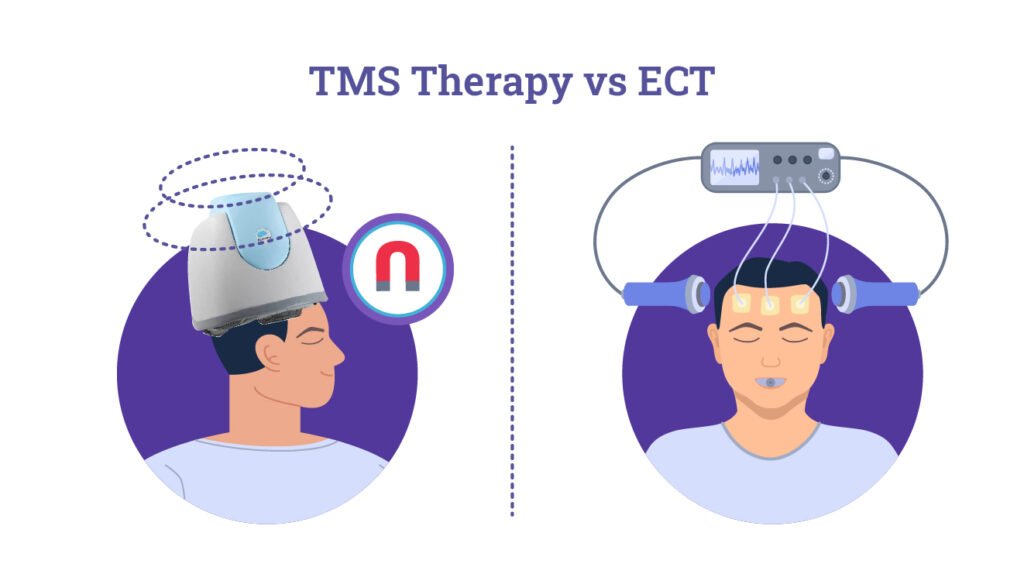
TMS vs. ECT: Understanding the Differences
Mental health conditions such as severe depression can sometimes be difficult to treat with medications and psychotherapy alone. For patients who do not respond adequately to conventional treatments, brain stimulation therapies can offer significant relief. Two of the most widely used treatments in this category are Transcranial Magnetic Stimulation (TMS) and Electroconvulsive Therapy (ECT). Read out the article to know the key differences at TMS vs ECT.
Although both therapies aim to improve brain function and treat psychiatric disorders, they work in very different ways. They differ in their mechanism of action, procedure, side effects, recovery time, and patient experience.
Understanding these differences helps patients and families make informed decisions about treatment options. In Faridabad, Dr. Kunal Bahrani, known as the Best Neurologist for Transcranial Magnetic Stimulation (TMS) in Faridabad, offers advanced neurological therapies including TMS for patients suffering from treatment-resistant depression and related conditions.
This guide explains how TMS and ECT differ, their benefits, potential side effects, and which patients may benefit from each treatment.
What Is Transcranial Magnetic Stimulation (TMS)?
Transcranial Magnetic Stimulation (TMS) is a non-invasive brain stimulation therapy that uses magnetic pulses to stimulate specific regions of the brain associated with mood regulation.
During the procedure, a specialized electromagnetic coil is placed on the patient’s scalp. The device generates repetitive magnetic pulses that stimulate nerve cells in targeted brain areas.
These pulses help improve communication between brain cells and restore normal activity patterns, particularly in patients with depression.
One of the key advantages of TMS is that it does not require anesthesia, sedation, or hospitalization, making it a convenient outpatient treatment.
What Is Electroconvulsive Therapy (ECT)?
Electroconvulsive Therapy (ECT) is a medical treatment that uses controlled electrical stimulation to induce a brief seizure in the brain. The procedure is performed under general anesthesia with muscle relaxants to ensure patient safety and comfort.
ECT has been used for several decades and remains one of the most effective treatments for severe psychiatric conditions, especially when rapid improvement is required.
The controlled seizure triggered during ECT leads to chemical and functional changes in the brain, which can significantly improve symptoms of severe depression and other mental health disorders.
Despite misconceptions, modern ECT is highly controlled and performed under strict medical supervision.
Mechanism of Action: How TMS and ECT Work
Although both therapies affect brain activity, the mechanisms involved are very different.
TMS Mechanism
TMS works by delivering magnetic pulses to stimulate nerve cells in specific brain regions.
Key characteristics include:
- Uses electromagnetic coils placed on the scalp
- Induces small electrical currents in targeted brain areas
- Does not cause seizures
- Does not require anesthesia or sedation
The treatment gradually modulates neural circuits responsible for mood regulation, helping improve depressive symptoms.
ECT Mechanism
ECT works by triggering a controlled seizure in the brain using electrical stimulation.
Key characteristics include:
- Electrical currents are delivered through electrodes placed on the scalp
- A brief seizure is intentionally induced
- Procedure is performed under general anesthesia
- Muscle relaxants prevent physical convulsions
The seizure activity leads to neurochemical changes in the brain, which can quickly relieve severe psychiatric symptoms.
Side Effects Compared
Both TMS and ECT are considered safe when performed by experienced specialists. However, their side effect profiles differ significantly.
TMS Side Effects
TMS is generally well tolerated with minimal side effects.
Common side effects include:
- Mild headache
- Scalp discomfort at the treatment site
- Tingling sensation during stimulation
These symptoms are usually temporary and resolve quickly.
Importantly, TMS does not cause memory loss or cognitive impairment, which makes it attractive for many patients.
ECT Side Effects
ECT may produce stronger side effects due to the use of anesthesia and seizure induction.
Common side effects include:
- Temporary memory gaps
- Confusion after treatment
- Headache
- Muscle soreness
- Fatigue after anesthesia
Memory disturbances are typically short-term, though some patients may experience longer-lasting memory issues.
Because of these effects, patients undergoing ECT usually require recovery time after each session.
Use Cases: When Each Therapy Is Recommended
Both treatments are effective, but doctors recommend them for different clinical situations.
When TMS Is Used
TMS is often recommended for patients who have:
- Treatment-resistant depression
- Difficulty tolerating antidepressant medications
- Moderate to severe depression without psychotic features
- Anxiety or OCD (in selected cases)
TMS is especially helpful for patients who prefer a non-invasive, medication-free treatment option.
When ECT Is Used
ECT is usually recommended in more severe situations such as:
- Severe or life-threatening depression
- Depression with suicidal risk
- Catatonia
- Severe bipolar disorder
- Psychotic depression
ECT is often chosen when rapid symptom relief is critical, such as when patients are unable to eat, sleep, or function normally.
Patient Experience: Comfort and Recovery
One of the major differences between TMS and ECT is the patient experience during and after treatment.
TMS Patient Experience
TMS sessions are straightforward and comfortable.
Patients typically:
- Sit in a comfortable chair
- Remain awake and alert
- Experience mild tapping sensations on the scalp
Each session lasts 20–40 minutes, and patients can immediately return to work or daily activities afterward.
TMS treatments are usually scheduled five days per week for several weeks.
ECT Patient Experience
ECT requires more preparation and monitoring.
Patients must:
- Fast before the procedure
- Receive general anesthesia
- Be monitored during recovery
After treatment, patients may experience temporary confusion or drowsiness, and someone may need to accompany them home.
ECT sessions are usually performed two to three times per week over several weeks.
Addressing Stigma Around Brain Stimulation Therapies
Unfortunately, both TMS and ECT have faced misconceptions and stigma, often due to outdated portrayals in media.
Modern treatments are highly advanced, safe, and carefully regulated.
Doctors carefully evaluate each patient to determine the most appropriate therapy based on their medical condition, treatment history, and overall health.
Education and awareness are important in helping patients understand that these therapies are effective medical treatments designed to improve quality of life.
Why Expert Guidance Matters
Choosing the right therapy requires a personalized evaluation by an experienced neurologist or mental health specialist.
Factors that influence treatment decisions include:
- Severity of depression
- Response to previous treatments
- Medical history
- Patient preferences
- Risk factors
In Faridabad, Dr. Kunal Bahrani, widely recognized as the Best Neurologist for Transcranial Magnetic Stimulation (TMS) in Faridabad, offers advanced evaluation and treatment for patients struggling with neurological and mood disorders.
With expertise in modern neuromodulation therapies, he helps patients find safe and effective treatment strategies tailored to their needs.
Conclusion
Both Transcranial Magnetic Stimulation (TMS) and Electroconvulsive Therapy (ECT) are powerful brain stimulation treatments that can significantly improve symptoms of depression and other psychiatric conditions.
However, they differ in several important ways. ECT involves controlled seizure induction under anesthesia and is typically used for severe psychiatric conditions, while TMS uses targeted magnetic stimulation without anesthesia and is commonly used for treatment-resistant depression.
Each therapy has its own benefits, risks, and indications. The best treatment option depends on the patient’s medical condition, treatment history, and severity of symptoms.
Consulting an experienced specialist like Dr. Kunal Bahrani, the Best Neurologist for Transcranial Magnetic Stimulation (TMS) in Faridabad, can help patients understand their options and choose the most suitable treatment for long-term mental wellness.
Frequently Asked Questions (FAQs)
- Is TMS safer than ECT?
Both treatments are safe when performed by trained specialists. However, TMS generally has fewer side effects and does not require anesthesia.
- Does TMS cause seizures like ECT?
No. TMS does not induce seizures. It uses magnetic pulses to stimulate brain cells without triggering seizure activity.
- Which treatment works faster?
ECT often produces faster results in severe depression, while TMS usually requires multiple sessions over several weeks for gradual improvement.
- Does ECT cause memory loss?
ECT may cause temporary memory gaps or confusion, but these effects are usually short-term.
- Can I go to work after TMS therapy?
Yes. Since TMS is an outpatient procedure without sedation, patients can resume normal activities immediately after treatment.
- Is TMS painful?
No. Most patients feel only mild tapping or tingling on the scalp during the treatment.
- Who is a good candidate for TMS therapy?
Patients with treatment-resistant depression or those who cannot tolerate antidepressant medications may benefit from TMS.
- How many sessions are required for TMS?
Most treatment plans include 20–30 sessions over 4–6 weeks, depending on individual response.